Treatment
Many cases of mild to moderate chondromalacia patella can be
treated with just oral anti-inflammatory medication, weight
loss and the proper type of therapeutic exercise. While nutritional
supplements such as glucosamine and chondroitin have been
shown to ease arthritic joint discomfort and slow down articular
cartilage breakdown in some patients, there is no convincing proof
yet that they totally halt or reverse chondromalacia. Viscosupplementation
(Synvisc, Hyalgan, etc.) injection treatment does not seem to
work as well on patellar arthritis pain as it does on symptoms
caused by arthritic joint surfaces elsewhere in the knee.
 |
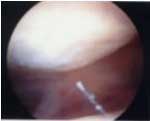
| FIGURE 1
- Arthroscopic photograph of fairly advanced chondromalacia
afflicting the gliding surface cartilage behind the patella
(top section of photo). Unlike what you see here, the surface
of the patella is normally quite smooth. |
If patellar cartilage deterioration proceeds beyond simple softening
and involves fissuring, disintegration and/or outright erosion
(see FIGURE 1), the joint surface
can become quite irregular and a sensation of grinding or catching
may be felt by the patient when extending (straightening) the
knee. This is often more pronounced when ascending stairs, or
when getting back up from a bent-knee (squat) position. Such symptoms
can often be improved by surgery.
During an arthroscopic "chondroplasty"
procedure the roughened and degenerated articular cartilage
tissue behind the patella is shaved down, re-contoured and evened
out to the maximum extent possible or practical, using arthroscopic
instruments (see FIGURE 2). Laser
or radio frequency (r.f.) electro-thermal ablation "sculpting"
techniques can also be employed, but extreme care must
be taken not to allow excessive heat build-up within nearby healthy
cartilage or the underlying bone, as this can cause localized
cartilage coagulation, or worse, bone death (avascular necrosis),
with potentially catastrophic results. I once encountered a patient
treated by another surgeon, in whom a simple, outpatient laser
chondroplasty resulted in enough bone death within the patella
to ultimately require its complete surgical removal (patellectomy)!
 |
|
FIGURE
2 - Photograph of a deteriorated patellar surface
after arthroscopic shaving. While not restored to normal,
a firmer, more even gliding surface has been created and
the patient should have less pain and experience less patellar
grinding/catching sensations.
|
If arthroscopy is performed to treat a deteriorated patellar
articular cartilage surface, concomitant surgical release (division)
of the lateral retinaculum is often (but not always) appropriate.
A retinacular release can be done from inside the knee
using an arthroscope. In cases of extensive chondromalacia combined
with poor patellar alignment and/or patellar instability, extensive
patellar realignment surgery is sometimes needed. This may involve
lower thigh muscle/tendon transfers and/or some "carpentry"
on the upper tibia ("shin bone") to redirect the angle
at which the patellar tendon pulls on the patella.
After patellar surgery a patient's knee and leg may temporarily
behave as if they are "in shock". The knee joint may
remain swollen and irritable for quite some time, and the leg
may lose quite a bit of thigh muscle tone and strength. Sometimes
special physical therapy regimens that involve electrical muscle
stimulation and biofeedback are required to gradually "re-educate"
the dysfunctional leg muscles, teaching them how to contract fully
again so that they may then be strengthened through routine resistance
exercise. Despite such difficulties, if a patient's knee
pain is alleviated by the surgery, near-complete restoration of
muscle function may be possible following a diligent rehabilitation
regimen.
Arthroscopic treatment of chondromalacia patella, with or without
lateral retinacular release or other more major procedures, can
produce gratifying results, but does not represent a total "cure"
for the problem. Once articular cartilage has become degenerated,
simply shaving away the worst of it does not really restore a
joint to normalcy. Sometimes the procedure is palliative, at best,
and subsequent surgery and/or specialized brace treatment may
be needed. Despite recent advances in surgery, physical therapy,
medications and knee bracing, the problem of the stubbornly painful
patellofemoral joint is one that orthopedic surgeons have yet
to solve, short of prosthetic joint replacement.
|