Natural History and Diagnosis of OCD
OCD lesions may or may not cause symptoms early
on. They apparently first appear in the early part of adolescence,
well before skeletal maturity is reached and the child's "growth
plates" fuse (close). Prior to fusion of
the growth plates, if the lesion remains undisturbed (i.e.,
does not loosen or separate), the chance for spontaneous healing
by way of natural reunification of the abnormal subchondal ossicle
with the parent bone is reasonably high. In patients between 10
and 13 years of age, simple rest and avoidance of stress to the
knee joint over a period of time may be enough to allow such natural
healing to take place. As skeletal maturity approaches, the chances
for spontaneous healing diminish, and the probability that surgical
treatment of some type will be needed increases
Some undetected cases of OCD remain unhealed and clinically
silent (cause no symptoms) until a patient reaches their
twenties and sometimes even their thirties or later. Some patients
can harbor a fairly large osteochondritis dissecans lesion in
their knee without realizing it until it frankly separates and
literally pops loose inside their joint! Separation may occur
either gradually, or all at once during a mildly stressful event
such as a routine pivoting or turning maneuver. In a teenager
or young adult, the sudden onset of knee locking or internal "clunking"
followed by joint swelling (without having experienced the degree
of knee stress usually required to tear healthy ligament or cartilage
tissues) should suggest to an examining physician the possibility
of a recently loosened or separated osteochondritis dissecans
lesion. OCD is notoriously misdiagnosed and underdiagnosed,
particularly in adolescents whose lesions have not yet separated.
These patients usually experience only vague symptoms and may
have no knee swelling whatsoever. Routine x-rays ordered by pediatricians
may not include the special views necessary to see an osteochondritis
dissecans lesion clearly, leaving it to go untreated and thus
possibly loosen and separate later on. Unless an MRI scan or the
appropriate x-rays are ordered, it usually takes an orthopedic
surgeon to make the diagnosis. A scene that has recurred many
times in my office is a 15 or 16-year-old patient (who had voiced
vague complaints to skeptical parents over several years) saying,
"See, there really was something wrong with my knee!"
By then, however, surgery is almost always needed.
The potential adverse consequences of osteochondritis dissecans
depend very much upon the size of the lesion, its location and
how amenable it is to "restorative" treatment. Restorative
treatment leads to healing of the lesion, with preservation of
the weight-bearing joint surface. Small lesions in non-critical
regions of the tibial joint surface and patella
often have a fairly benign clinical course, even when the only
treatment possible is removal of the loose osteochondral fragment
from the joint, which leaves a defect in the articular surface.
Unsuccessfully restored femoral condylar lesions are more
likely to cause arthritis over time.
Large, advanced lesions of the femoral condyles that are fragmented
or otherwise not amenable to restorative treatment leave substantial,
crater-like defects in the main weight-bearing surface of the
knee joint, with almost uniformly poor long-term results. Such
a knee behaves like a ball-bearing with a large divot in its surface,
essentially wearing itself out prematurely. Some varieties of
femoral osteochondritis dissecans involve a fairly extensive zone
of abnormal, underlying subchondral bone. These leave a deep crater
if the lesion loosens and separates. Other varieties of OCD extend
only superficially into the underlying subchondral bone. In all
cases that do not heal spontaneously, the patient's body forms
a zone of fibrous tissue between the parent bone and the OCD fragment.
This fibrous interface layer is relatively inert
(inactive) tissue. The few living cells within this fibrous tissue
try to absorb the dead bone in the overlying OCD fragment, which
thickens the fibrous tissue layer as the adjacent bone dissolves.
Because fibrous tissue is soft, this makes for a loss of structural
support beneath the OCD lesion (see FIGURE
3).
|
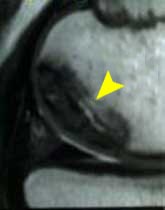
FIGURE
3 - This MRI image scan shows a side-view close-up
of the rear portion of a femoral condyle afflicted with
a large osteochondritis dissecans lesion (arrow). The black
triangular structure immediately below the OCD lesion represents
a cross section of the patient's normal meniscus (the so-called
"knee cartilage"), with the tibia being located
immediately below that. At the junction of the dark OCD
lesion and the lighter-shaded normal bone of the main femoral
condyle, the structurally weak, fibrous interface zone can
be seen. This is where a lack of underlying joint surface
support develops, allowing repetitive, pistoning micro-motion
of the OCD lesion under the weight-bearing stresses of daily
activity. This is similar to the way floorboards will move
when you step on them if the underlying framing is weak.
If you look closely at the lower, far right end of the OCD
lesion, you can see a short black line. This represents
an early dissection fissure developing through the articular
surface cartilage covering the femoral condyle. Such fissures
typically develop along the outer perimeter of OCD lesions,
gradually separating them from their parent bone.
|
 |
This lack of underlying support allows the cartilaginous
joint surface to flex repeatedly under weight-bearing stresses,
much like floorboards with weak support framing beneath them.
Such repetitive, abnormal micromotion causes fatigue breakdown
of the articular (surface) cartilage along the lesion's perimeter
(the border interface between the OCD fragment and the surrounding,
structurally stable femoral surface), culminating in an open crack
or fissure demarcating some or all of the lesion. As noted previously,
this is the "dissection" process that gave OCD the last
part of its name.
If the ossific (bone tissue) nucleus of the OCD lesion shrinks
substantially in size, the entire lesion may weaken and break
apart (see FIGURE 4), thus precluding
any attempt at direct surgical repair and reunification (healing
by way of incorporation back into the parent bone).
|
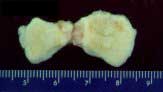
FIGURE
4 - This photograph shows fragments of an OCD lesion
that were removed from a young patient's knee joint. The
patient's lesion went untreated until it loosened and then
literally broke apart into several pieces, precluding their
replacement back into the crater that was left in the femoral
condyle. What you see here is the back side of the OCD fragments,
with the yellowish tissue being what was left of the underlying
bone and the white tissue behind the bone representing the
overlying articular (joint surface) cartilage. The measurement
scale shown is in centimeters. .
|
 |
|