Treatment of PVNS
The most commonly performed treatment for diffuse, pigmented
villonodular synovitis is a surgical synovectomy.
Synovectomy simply means removal of the internal joint lining
membrane. Before arthroscopic techniques were available, synovectomy
was performed in an open fashion, with a large frontal incision
literally opening the knee up like a book so that the majority
of the joint lining tissue, which is in the front of the joint,
could be stripped out. Opening up the rear of the knee to remove
the synovial lining in the back of the joint was sometimes done
as a more radical extension of the frontal synovectomy procedure.
These open surgical procedures had serious drawbacks, in that
they were quite painful and often produced major post-operative
morbidity such as joint scarring and stiffness. In addition, as
extensive as these procedures were, every last bit of abnormal
synovial tissue was still not removed. As noted
previously, to perform a genuinely complete surgical synovectomy,
extreme damage to the joint would have to be done because the
knee cartilages (menisci) would effectively have to be removed,
along with portions of the internal (cruciate) ligaments. Only
such radical surgery would allow access to all of the small nooks
and crannies within the knee joint where PVNS tissue can hide.
While not necessarily more effective than open synovectomy, in
most cases a better approach is arthroscopic synovectomy
(see FIGURE 4).
 |
FIGURE
4 - When removing PVNS tissue from the knee joint arthroscopically,
a small, motorized tissue resection instrument is introduced
into the knee through a 1/4 inch skin incision, or "portal."
The surgical work is observed by way of an arthroscope (shown
here in the upper right-hand section of the FIGURE), inserted
through another skin portal incision from a different angle.
Each pair of portal incisions (arthroscope and resector instrument)
allows a certain region of the knee joint to be cleaned out,
with a comprehensive synovectomy requiring upwards of six
to eight access portals |
For patients interested in the technical aspects of arthroscopic
knee synovectomy, reprints of my illustrated surgical technique
paper, published in Master Techniques in Orthopedic Surgery,can
be obtained by either writing or e-mailing our Knee and Shoulder
Centers office. Simply stated, the objective of arthroscopic
synovectomy is to remove as much abnormal joint lining tissue
as is technically feasible without damaging the patient's knee
in the process. Properly and meticulously performed, it is
a very lengthy and technically difficult surgical procedure. It
requires mastery of almost every knee access technique ever devised
by arthroscopic surgeons. All of the major internal regions of
the knee joint, in sequence, must be both visualized and accessed
by surgical re-section instrumentation, all the while keeping
the number of access (arthroscope portal) incisions to a minimum
and avoiding unintended neurovascular injury or damage to other
internal joint structures. The surgeon must be comfortable working
in the posteromedial and posterolateral knee compartments (see
FIGURE 5) and have the patience to follow the abnormal
joint lining tissue down into every accessible fold and recess
elsewhere within the knee joint. When PVNS disease afflicts the
cruciate ligaments, the synovial lining membrane of these ligaments
must be carefully and meticulously dissected away (both in the
front and sometimes in back) without damaging the ligaments themselves
(see FIGURE 6).
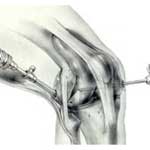 |
FIGURE
5 - This illustration shows another step during the
course of a comprehensive, internal knee synovectomy. Here,
the arthroscope (left) is being inserted into the posterolateral
(rear, outside) compartment of the knee directly, while the
resector instrument reaches the inner regions of that compartment
indirectly by passing through the inter-condylar notch (center
space of the knee) from the front. When creating surgical
access portals toward the back side of the knee, great care
must be taken not to injure the nearby nerves and blood vessels
leading to the lower leg. In this picture, the critically
important peroneal nerve is seen just beneath the posterolateral
arthroscope access portal. Remember that the surgeon cannot
actually see this nerve at the time the adjacent skin portal
incision is made! He or she must be guided by way of external
landmarks and a sound knowledge of internal knee anatomy. |
|
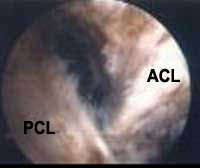
FIGURE
6 - This arthroscopic view demonstrates a patient’s
anterior cruciate ligament (ACL) and posterior cruciate
ligament (PCL), looking from behind, as the arthroscope
has been inserted by way of a posterior-medial portal access
site. These cruciate ligaments were previously surrounded
by PVNS tissue, which was carefully stripped away, both
in front and in back, by way of arthroscopic instrumentation.
|
 |
Clinical experience has generally demonstrated that the more
complete the degree of synovectomy achieved, the lower the recurrence
rate of the disease. However, even with a consummately skilled
surgeon using the most advanced arthroscopic techniques, it is
still impossible to remove every last bit of PVNS tissue in the
diffuse form of the disease. Current surgery is, therefore, limited
to a thorough "debulking"process that falls short of
total resection. The surgeon attempts to achieve the greatest
possible debulking effect in order to minimize the recurrence
rate,while still leaving the patient with a functional knee afterwards.
Why the disease does not recur in all cases, following what
we know to be less than a 100% synovectomy, is unknown. Diffuse
PVNS is truly a strange disease that appears for uncertain reasons
and may also completely exit a patient's life following treatment,
even though by definition that treatment is known to have been
incomplete. If there has been any common etiologic
(causal) thread in many of the PVNS patients I have treated, it
has been that they had some episode of knee trauma in their past
that caused bleeding within their knee joint. Whether a brief
exposure of a synovial joint to the iron-based hemoglobin pigment
released by degrading red blood cells can actually cause PVNS
has never been proven and at this point must be relegated to personal
speculation.
Other means of treating pigmented villonodular synovitis include
radiation beam therapy and radio isotope synovectomy. In the latter
procedure a liquid, radioactive isotope is injected into the knee
joint, subjecting the synovial lining to radiation treatment.
This is an uncommon treatment that in the past has generally been
reserved for difficult cases of PVNS that have recurred following
a prior surgical synovectomy. Very few medical centers in the
United States even offer such treatment, which is usually done
under carefully controlled conditions in research protocols. Either
form of radiation therapy can also be used as an adjuvant (additional
or back-up) treatment following a surgical synovectomy.
If PVNS remains uncontrolled, over a period of years the patient's
knee joint surfaces may gradually become destroyed, leading to
a need for radical joint resection and replacement by prosthetic
components ("total knee replacement" surgery). The initial
radical resection stage of such a procedure allows relatively
complete exposure inside the joint and thus an unusually complete
surgical synovectomy. This often leads to a final cure of the
disease, but the original knee joint has been lost forever.
In this author’s experience, a recurrence of diffuse PVNS
following an initial synovectomy procedure is still worth treating
with another attempt at a comprehensive arthroscopic synovectomy,carried
to the most radical extent that is feasible. In some cases unusual
measures such as resecting the soft tissue from behind the posterior
cruciate ligament must be performed, as that is a site where nests
of PVNS tissue may form and even begin to reach outside the
confines of the knee capsule. Resection of such extra capsular
(outside of the knee joint proper) PVNS tissue with an arthroscope
is an extremely tricky process, particularly in the posterior
regions of the knee joint where the major neuro vascular structures
that feed the lower leg and foot are located. Most scientific
articles and book chapters on PVNS do not even discuss the fact
that PVNS tissue can occasionally escape the confines of the joint
cavity to invade soft tissues outside of the capsule. While it
is well known that PVNS tissue can actually grow into the femur
or tibia itself, apparently by following vascular (blood vessel)
channels into the bone, it is less commonly appreciated that PVNS
tissue can grow along small, trans-capsular passage ways leading
out of the knee joint cavity to form masses of tissue in external
regions. Two such regions are known as the lateral popliteus recess
and the medial gastrocnemius-semimembranosus bursa (see
FIGURE 7). Extra-capsular extensions of PVNS disease are
best detected pre-operatively by way of MRI scanning with special,
hemosiderin-weighted imaging techniques. If identified, such extra-articular
nests of PVNS tissue are usually best resected by way of localized,
open surgical exploration, leaving the intra-articular PVNS tissue
to be resected by arthroscopic means.
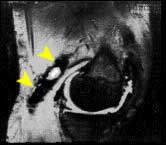 |
FIGURE
7 - This MRI scan shows a cross-sectional, side view
of a knee. The rounded femoral condyle sits atop the flat
upper tibia. The front of the knee is to the right and the
back of the knee is to the left. The arrow points to an accumulation
of PVNS tissue outside of the knee joint, filling up a natural
pouch or space known as the gastrocnemius-semimembranosus
bursa. The PVNS tissue appears black in this MRI study. If
you look within the knee joint cavity in front of the femur,
you will see additional, dark PVNS tissue, in a more typical
location. This patient was treated with a comprehensive arthroscopic
synovectomy inside the joint followed by excision of the extra-articular
mass of PVNS tissue (arrow) using an open, posteromedial skin
incision and exploration. Six years after surgery, this patient
was symptom free and an apparent cure. |
Resolution of the disease process is usually heralded by an elimination
of the patient's prior recurrent knee effusions (excess joint
fluid accumulations). Post-operative MRI scans are extremely
difficult to read because of scar tissue artifact. If at some
point excess knee joint fluid begins to return, this is suggestive,
but not definitive proof of, recurrence. If long-lasting, the
presence of recurrent fluid suggests the need for a follow-up
MRI scan and an arthroscopic re-inspection of the joint.
For recurrent disease, a combination of repeat synovectomy,
possibly followed by irradiation or radioisotope, adjuvant
synovectomy, can be considered. Individual consultation between
the patient and the subspecialists at those few medical centers
offering the latter technique is required to determine whether
the patient is a potential candidate for this treatment.
|