

|
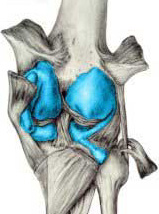
Pigmented villonodular synovitis, or PVNS, is an uncommon but not necessarily rare disease that affects the internal lining membrane of the body's moving joints. Large joints are the most commonly afflicted, with the most frequent site being the knee. Joints where movement occurs between one or more bones always have a surrounding envelope of ligament tissue (capsule) that is lined internally by a thin, soft tissue membrane (colored in blue, see FIGURE 1)comprised of synovial cells. This synovial membrane secretes the lubricating (synovial) fluid that keeps friction between its gliding, cartilaginous surfaces of joints to an absolute minimum. A youthful, normally functioning synovial joint generates less friction than one smooth piece of ice gliding upon another! For unknown reasons, some or all of the synovial lining tissue of a joint occasionally undergoes a change and becomes diseased, wherein the joint lining tissue becomes thick and overgrown and accumulates a rust-colored, iron pigment known as hemosiderin. Strange, foamy cells and large (so-called "giant") cells with many nuclei also appear. The overgrowth of the joint lining tissue can occur diffusely throughout a joint by way of a generalized thickening of the entire lining membrane, or a localized area of synovial membrane can overgrow and form a discrete nodule (tissue mass) that remains attached to the rest of the internal joint lining by way of a stalk. While this disease process does involve abnormal tissue growth, it is uniformly benign and has not been known to metastasize as do malignant growths. PVNS can be considered a benign, "neoplastic" (tumor growth) process, with some varieties being more aggressive in their growth and thus harder to treat, and other varieties being less aggressive in their growth and thus easier to treat. Medical pathology textbooks generally describe two forms of PVNS. The localized form is called "nodular" PVNS. The non-localized form is referred to as "diffuse" PVNS. While this author has never found an "in-between" variety referenced in any textbook, I have seen and treated cases that appeared to represent a mixed (diffuse and nodular) form of the disease.
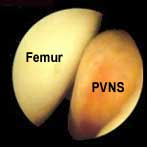
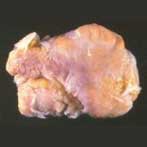
The localized (nodular) form of PVNS is generally the least difficult to treat, as all of the abnormal tissue growth is located in a single, excisable mass within the joint (see FIGURE 2a). It is usually painless and often does not become noticed until the tissue nodule reaches a size that causes swelling or some type of internal joint impingement symptoms to the patient. Obvious mechanical problems such as joint locking and snapping can occasionally occur, simulating a torn cartilage or other structural problem. On other occasions, the patient may simply feel a slowly growing soft tissue mass within their knee joint and/or their knee may become distended with excess synovial fluid (so-called "water on the knee"). MRI scanning is the best non-invasive means of identifying the presence of a synovial growth within a joint. Treatment is usually rendered both simply and effectively by way of either arthroscopic or "open"(access by way of a traditional incision) resection of the abnormal tissue (see FIGURE 2b).
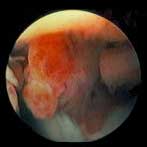
The diffuse form of pigmented villonodular synovitis is more problematic. The synovial lining everywhere within the large, complex multi-compartmental knee joint becomes overgrown, sometimes taking on a rust-colored, "bearded" appearance (see FIGURE 3). Every tiny nook and cranny within the knee joint may be afflicted, making it impossible to surgically eliminate every last bit of abnormal tissue without literally destroying the knee and its surrounding capsule in the process. For this reason and perhaps others, the diffuse form of PVNS is much more likely to recur (relapse) following attempted surgical resection than the nodular form. Almost nothing is known about the mixed form, but in this author's opinion it is probably best viewed as a variety of the diffuse form of the disease, given that the nodules are small and interspersed amongst diffuse synovial lining overgrowth.
One thing that the diffuse form of PVNS has in common with the nodular form is that it is often misdiagnosed initially. The former may be even harder to diagnose than the latter because it does not have a discrete, nodular soft tissue mass as its calling card. Diffuse PVNS is almost always an entirely painless disease, at least in its early stages, and it most commonly presents itself as simple knee swelling caused by an excessive accumulation of synovial fluid within the joint. This excess fluid is secreted by the overgrown joint lining tissue. Unless the quantity of fluid in the joint becomes so great as to stretch the joint capsule and cause discomfort, patients often regard this as more of an annoying curiosity than a significant problem at first. Patients who present for medical evaluation find that their knee x-rays are almost always normal and that all of their blood tests are negative for diseases like rheumatoid arthritis, lyme disease, lupus, etc. Clinicians should always keep in mind the possibility of PVNS when presented with a patient who is suffering from unexplained, recurrent fluid accumulations in one of their joints, especially when the joint fluid has a slightly more orange-brown color to it than normal. Sometimes the delicate, overgrown joint lining tissue bleeds intermittently and thus even red joint fluid may be found at times. The presence of diffuse PVNS is verified by direct arthroscopic inspection of the interior of the joint and taking a synovial tissue biopsy. Microscopic tissue analysis is required to make a firm pathologic diagnosis. Once this has been confirmed, treatment must be planned. |