
|
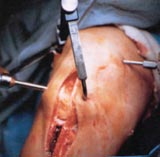 |
FIGURE 7a - This photo demonstrates the patellar tendon autograft method of ACL reconstruction, whereby the middle 1/3 of this frontal knee tendon, with a bone plug at either end, is first excised and then re-implanted inside the knee where the ACL originally was. The defects in the patellar tendon, patella and tibia left from the graft "harvesting" procedure gradually fill in with scar and repair tissue. |
 |
FIGURE
7b - Diagrammatic illustration of how a patellar tendon
graft is surgically implanted into the knee where the original
ACL was located. Two screws hold the (bone plug) ends of the
new ACL in place. |
In our experience, this surgical method poses a higher risk for unwanted side-effects such as patellar tendinitis, patellar pain, joint stiffness, internal scarring, and an inability to kneel on firm surfaces (any or all of which could be permanent). For this reason, we view this particular procedure as being more ideally suited to younger (under 25), high-demand athletes who are not likely to be called upon to kneel on hard surfaces in an occupational setting. Patellar tendon autograft ACL reconstruction, done in the wrong patient, has a significant chance of leading to an unhappy result. We are of the opinion that an individual over 25 with an acute (recent) anterior cruciate ligament injury that has not yet resulted in a highly unstable joint, and who later may be required to do more kneeling activity in an occupational setting than cutting or pivoting in an athletic environment, is better suited for other methods of anterior cruciate ligament reconstruction. These alternate methods utilize either two of the patient's own accessory hamstring tendons (semitendinosus and gracilis) as an ACL graft (see FIGURE 8), a part of the patient's own quadriceps tendon from the front of the lower thigh, or an allograft tendon specimen obtained from a tissue bank (see FIGURE 9).
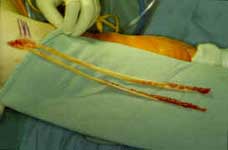 |
FIGURE 8 - This photo demonstrates how two accessory (thus relatively expendable) hamstring tendons can be retrieved from the thigh through a 1½ inch long incision, made just below the knee. These tendons are then doubled or tripled-over, and fashioned into an ACL graft that is arthroscopically implanted into the knee at the site where the original ACL was located. |
|
FIGURE
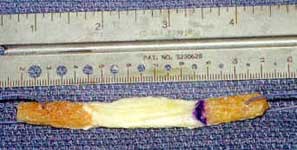
9 - Photo demonstrating an "allograft"
bone/patellar-tendon/bone specimen that has been obtained
from a certified tissue bank. The photo shows the specimen
after it has been cut down to size and fashioned into a
new ACL. The white, middle section becomes the new ligament
and the bone plugs at either end serve as anchors that become
imbedded in the femur and tibia.
|
 |
These alternate techniques leave the patient's own patellar tendon untouched and rarely produce sensitive areas in the front of the knee to be bothered later on by floor contact when kneeling. While there is no surgical knee procedure that poses zero risk of an unhappy or frankly failed outcome, these alternate methods are often better tolerated by many patients as compared with ACL reconstruction using their own patellar tendon.
There are also various specific technical advantages and disadvantages
to each particular surgical method and/or ACL graft when considered
in the context of a patient's exact clinical circumstances. Taking
into account these various details, educating the patient about
them and then jointly arriving at a decision as to how to proceed,
is our preferred approach to the problem of the ruptured anterior
cruciate ligament. Our goal is to subject a patient's knee
to no more surgical stress than is necessary to
achieve the desired result.