Surgical Treatment of Femoral OCD
In formulating a treatment plan for a patient
with an OCD lesion, the knee specialist's approach is first directed
at establishing whether the lesion is mechanically stable
or unstable (i.e., still firm and well-fixed in place vs. already
loose or frankly mobile). Sometimes, obvious clinical symptoms
or the initial x-ray findings (such as a loose piece of bone in
the joint) are a "give-away" in this regard. In less
obvious cases, the combination of x-rays, a bone scan, and
an MRI scan can predict the likelihood of stability versus instability
with perhaps a 75-80% accuracy. (For further information regarding
the value of such diagnostic screening tests in cases of osteochondritis
dissecans, reprints of my published research in this area are
available by writing or e-mailing the Knee and Shoulder Center).
Taking into account the patient's age and clinical symptoms, the
surgeon will interpret the results of these non-invasive diagnostic
tests and determine if an attempt at non-operative treatment is
reasonable, vs. recommending operative treatment.
The first step in the operative treatment of unstable lesions
or stable lesions that are deemed unlikely to heal on their own
is direct arthroscopic inspection. Even though the lesion may
be obvious on an MRI scan or x-ray, finding it within the joint
can be tricky if it has not yet become mobile. The overlying articular
surface cartilage may appear entirely normal, with perhaps the
lone exception of an extremely subtle contour irregularity at
the perimeter of the lesion. This can be very difficult to appreciate
visually with an arthroscope (see FIGURE
5). Probing the joint surface with firm pressure
administered by a blunt instrument may help the surgeon locate
the lesion by detecting micro-motion of the underlying bone fragment.
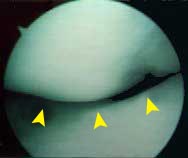 |
FIGURE
5 - As viewed with the arthroscope (femoral condyle
above and tibial articular surface below), OCD lesions that
have not overtly loosened or separated may actually be difficult
to locate. The arrows here point to a slight bulge in the
normal curvature of the femoral condylar surface, which in
this patient was the only visible sign of a very large, underlying
OCD lesion that was quite obvious on an MRI study. This patient
went on to have a retrograde bone grafting and screw fixation
procedure (see Figures 6 and 7), which resulted in complete
healing of the lesion before it ever had the chance to grossly
loosen or separate. |
One way of treating stable and relatively stable lesions is by
a drilling a number of small holes through the involved articular
surface, proceeding down through the OCD ossicle and fibrous tissue
interface into the normal bone of the parent femur. This is done
in the hope of creating internal bone bleeding and an inflammatory
healing reaction that ultimately fixes the underlying bone ossicle
into its crater (the two bone surfaces will hopefully "knit"
together, as would a fracture). This approach has the disadvantage
of potentially compromising the otherwise healthy, articular cartilage
cap over the OCD ossicle by way of the multiple, drill-hole punctures.
Another, more technically difficult approach is to perform "retrograde"
(coming in from behind) "bone grafting" of the lesion.
Bone grafting refers to a process where healthy bone tissue is
transplanted from an area where it is expendable, to an area where
bone is deficient and/or unhealed. The OCD lesion is approached
by drilling a small tunnel through the femur, starting at a distant
location and approaching the lesion from behind. The drilling
must stop just as the tunnel passes through the
lesion's fibrous interface layer, reaching the necrotic (dead)
OCD nucleus, or else the drill may go through the ossicle and
exit out through the articular surface cartilage, thus damaging
it. This procedure requires fluoroscopic (x-ray) guidance during
drilling (see FIGURE 6) and
direct visual confirmation that the fibrous interface has been
reached and breached by the drill bit. This is accomplished by
inserting the arthroscope directly down into the bone tunnel to
inspect its depths.
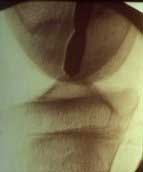 |
FIGURE
6 - This fluoroscopic x-ray taken during surgery demonstrates
a side-view of the same patient's knee as shown in Figure
5. Having located the OCD lesion within the femoral condyle,
special reference point markers and x-ray guidance were used
to drill a tunnel into the back side of the OCD lesion from
a remote location well away from the joint surface. The x-ray
demonstrates the furthest extent that the drill was inserted.
Once the drill was removed, a direct view down the bone tunnel
with the arthroscope confirmed that the tunnel had crossed
the fibrous interface layer and entered the ossific nucleus
of the OCD lesion. The bone tunnel was then packed with bone
graft to stimulate healing of the OCD lesion back to the parent
femoral condyle. |
A small amount of local femoral bone graft is then harvested
from an area near the tunnel entrance and pushed down to the bottom
of the tunnel. It is packed into the area where the fibrous tissue
interface layer previously existed. This creates a bone tissue
bridge between the ossific nucleus of the lesion and the parent
femur, hopefully allowing rigid, local bone-to-bone healing that
will spread and ultimately result in reunification of the entire
ossific nucleus to the parent femur without ever having disturbed
the overlying articular cartilage cap.
|
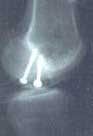
FIGURE
7 - X-ray of the same femoral condyle shown in Figure
5, after arthroscopic placement of fixation screws into
the OCD lesion had been performed. The screws were removed
ten weeks later and the OCD lesion was found to be firmly
healed and stable.
|
 |
For large lesions that are not completely stable but have not
yet developed overt perimeter fissuring of their articular surface
cartilage, the retrograde bone grafting technique can be supplemented
by internal fixation and stabilization of the fragment in situ
(right where it lies) by way of either removable, stainless steel
compression screws (see Figure 7)
or bioabsorbable (slowly dissolving) pins or compression screws.
This requires that one or two, very small holes be drilled through
the articular cartilage cap of the lesion for screw placement,
but this is still probably less traumatic to the joint than drilling
many holes through the cartilage cap, as is performed in a typical
anterograde (frontal approach) drilling procedure. The screws
hold the fragment rigidly in place to foster osseous union (healing
or "knitting") at the bone graft site. Non-absorbable
screws are typically removed after eight to ten weeks by way of
the arthroscope, and at that point the lesion can be probed and
checked for stability. If micromotion of the fragment is no longer
present, then early healing can be assumed to be taking place
and the patient can very gradually be allowed to resume weight-bearing
activities. During the time the screws are in place (assuming
proper screw position and grip), the patient can swim and bicycle
without harm to their knee, but they should not bear weight on
that leg. With absorbable screws a follow-up arthroscopy may not
be necessary, but this eliminates the chance for the surgeon to
check the early stability and healing of the lesion directly.
Because it takes a long time (six to twelve months) for healing
to be clearly recognizable by way of x-ray or an MRI scan, not
having the opportunity to recheck the patient's knee arthroscopically
leaves the surgeon with less information to go on when instructing
the patient with respect to their return to weight-bearing activities.
In cases where the OCD lesion is clearly unstable and the overlying
articular cartilage cap has begun to separate by way of circumferential
perimeter fissuring, a somewhat simpler (but still difficult to
perform) bone grafting technique can be employed wherein the bone
graft tissue is introduced arthroscopically into the OCD defect
from the front, as opposed to an indirect approach from behind
the lesion. Such lesions are often found incompletely separated,
hanging on by one area of articular cartilage or fibrous tissue
near the intercondylar notch (the central, open concavity in the
end of the femur). This acts like a hinge, allowing the lesion
to be flipped open as would a trapdoor, thus exposing the base
of the crater in the parent femur and the undersurface of the
un-united bone ossicle or cartilage cap (see
FIGURE 8).
|
|
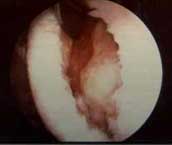
FIGURE 8
- Arthroscopic photo of a different patient whose femoral
OCD lesion had already experienced perimeter fissuring and
had become grossly loose. The underlying bone ossicle had
completely re-absorbed, leaving only a thick cartilage "cap".
The cartilage cap here is opening up on an unseen hinge
of partially intact surface cartilage, much like a "trap
door".
|
The surgeon will carefully hold the lesion open,scrape out any
fibrous tissue present (see FIGURE 9)
and then insert fresh local bone graft material into the crater
(see FIGURE 10). This bone graft
material must be very carefully inserted so as to fill up (but
not overfill) the empty space created by the removal of the fibrous
tissue. The OCD cap must then be closed back down and held in
place with internal fixation screws or pins before any of the
bone graft material escapes (see FIGURE
11). The greater the degree of prior reabsorption of the
dead ossific nucleus, the more fibrous tissue there is to remove
and the greater the amount of bone graft material required to
fill the void. One must be very careful not to overfill the crater
with bone graft or the cap will not fully close back down, causing
it to bulge out beyond the normal joint surface contour.
|
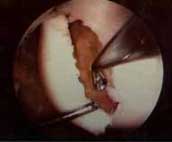
FIGURE
9 - With the cartilage cap (left side) held open to
expose the crater in the femur beneath it, the crater and
cap are scraped and cleaned of all fibrous tissue. Any dead
bone at the bottom of the crater is removed and/or drilled
to enhance restoration of local blood supply. |
|
|
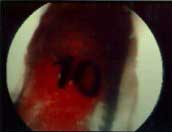
FIGURE
10 - This arthroscopic photo demonstrates how fresh
(red) bone graft material is inserted into a hinged-open OCD
lesion using a modified syringe (the clear plastic tube with
the "10" on it). This is a close-up view of the
same lesion depicted in Figures 8 and 9. The syringe is withdrawn
as the bone graft material is injected into the empty space
that remains after the previous removal of dead bone and fibrous
tissue. The articular cartilage cap is then closed back down
over the bone graft tissue, preventing its escape from the
crater. This cap was held in place with two fixation screws,
as shown in Figure 11. |
|
|
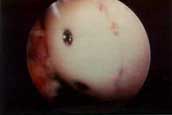
FIGURE 11
- This was the final appearance of the bone-grafted OCD
lesion shown in Figure 10, now held firmly in place with
two stainless steel screws. When the screws were removed
arthroscopically 10 weeks later, the OCD lesion was healed
and stable. The patient was able to run and perform heavy
weightlifting six months later with no symptoms of any kind.
|
In my experience I have come across two unusual OCD lesions
(one of which is shown above in FIGURES
8-11) where the entire ossific nucleus had
been reabsorbed, leaving only a thick cap of articular cartilage.
In both cases, bone grafting and internal fixation still successfully
resulted in firm union of the articular cartilage cap to the parent
femur and an ultimate clinical success. As of the time of this
writing, I have never encountered an OCD lesion that failed
to unite when bone grafting methods were employed, with or
without internal screw fixation of the lesion, as needed. Once
an individual with at least a partially unstable lesion has reached
skeletal maturity by way of closure of their growth plates, I
believe that non-operative treatment or less involved surgical
approaches (such as simple drilling) are less effective
than the more complex techniques utilizing arthroscopic bone grafting.
I have also not yet come across a case where bone grafting and
screw fixation of a lesion could not be done arthroscopically,
as opposed to opening up the knee by way of a large incision known
as an arthrotomy. Such arthroscopic procedures can be lengthy
and tedious, and somewhat akin to building a model ship in a bottle,
but the post-operative morbidity experienced by the patient (pain,
swelling, stiffness and scarring) is usually significantly less
and the cosmetic results to be obtained are superior to any procedure
that involves an arthrotomy (an important factor to many teenage
females).
If an OCD lesion comes completely loose, creating a free fragment
within the knee joint, the fragment should be carefully checked
with an arthroscope to see if it still has the appropriate size
and shape to fit back into its crater in the femoral condyle.
If so, then bone grafting and internal fixation methods should
be employed to try to replace the fragment in its bed and get
it to heal. If that is not feasible, then it must be removed from
the joint. The base of the empty crater can be abraded somewhat
to make it bleed and thereby provide for subsequent in-filling
by fibrocartilage (cartilage scar) tissue, but that almost never
provides a good weight-bearing surface and ultimately degenerative
joint arthritis will ensue. A possible salvage option in this
situation is packing bone graft material into such an open crater
to a level just slightly below the level of the surrounding surface
articular cartilage, hoping that a surface cartilage layer will
form over the solidifying bone graft. Another possible salvage
option in such a circumstance is to perform an "OATS"
(osteo-articular transplant surgery) procedure (see
FIGURES 12a-12d).
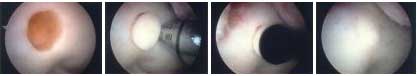 |
| FIGURES
12a-12d - An arthroscopic photo-series demonstrating
how an articular surface defect can be treated by Osteo-Articular
Transplantation Surgery (OATS). Here, a damaged zone of femoral
surface cartilage and a plug of bone beneath it are removed
and replaced by an identical sized plug of healthy surface
cartilage and underlying bone, harvested from an undamaged
donor (non-critical) area elsewhere in the same knee. The
final photo demonstrates the round, transplanted plug snugly
in place, a perfect fit. If the transplant "takes",
the treated area of joint surface has effectively been renewed.
|
During such surgery one or more plugs of healthy
articular cartilage and underlying subchondral bone are transplanted
from less important articular surface areas in the knee (donor
zones) to the open crater left by the osteochondritis dissecans
lesion, which usually occupies a more critical, weight-bearing
zone of the joint surface. Some surgeons are also using one or
more small OATS plug transfers as a substitute for the multiple
drill-hole or retrograde bone graft procedures mentioned earlier
for the treatment of stable, in situ OCD lesions.
It is worth remembering that the goal of each and every treatment
for osteochondritis dissecans is to preserve or restore a normally
contoured, well supported, weight-bearing articular cartilage
layer so that the gliding/load-bearing function of the joint surface
is not compromised. It is currently believed that success
in this regard will minimize the long-term development of degenerative
arthritis.
|